Did you know that a person with measles can be contagious for up to four days after the rash appears? Understanding this crucial window helps prevent the spread and protects your loved ones from this highly infectious disease. In this comprehensive guide, we clarify how long is a person contagious with measles after the rash appears, explore symptoms, prevention, public health strategies, and answer your most pressing questions with insights from real medical experts.
What You'll Learn About How Long a Person is Contagious with Measles After the Rash Appears
Key points about measles contagion timelines
The role of the rash in transmission
Prevention strategies and public health implications
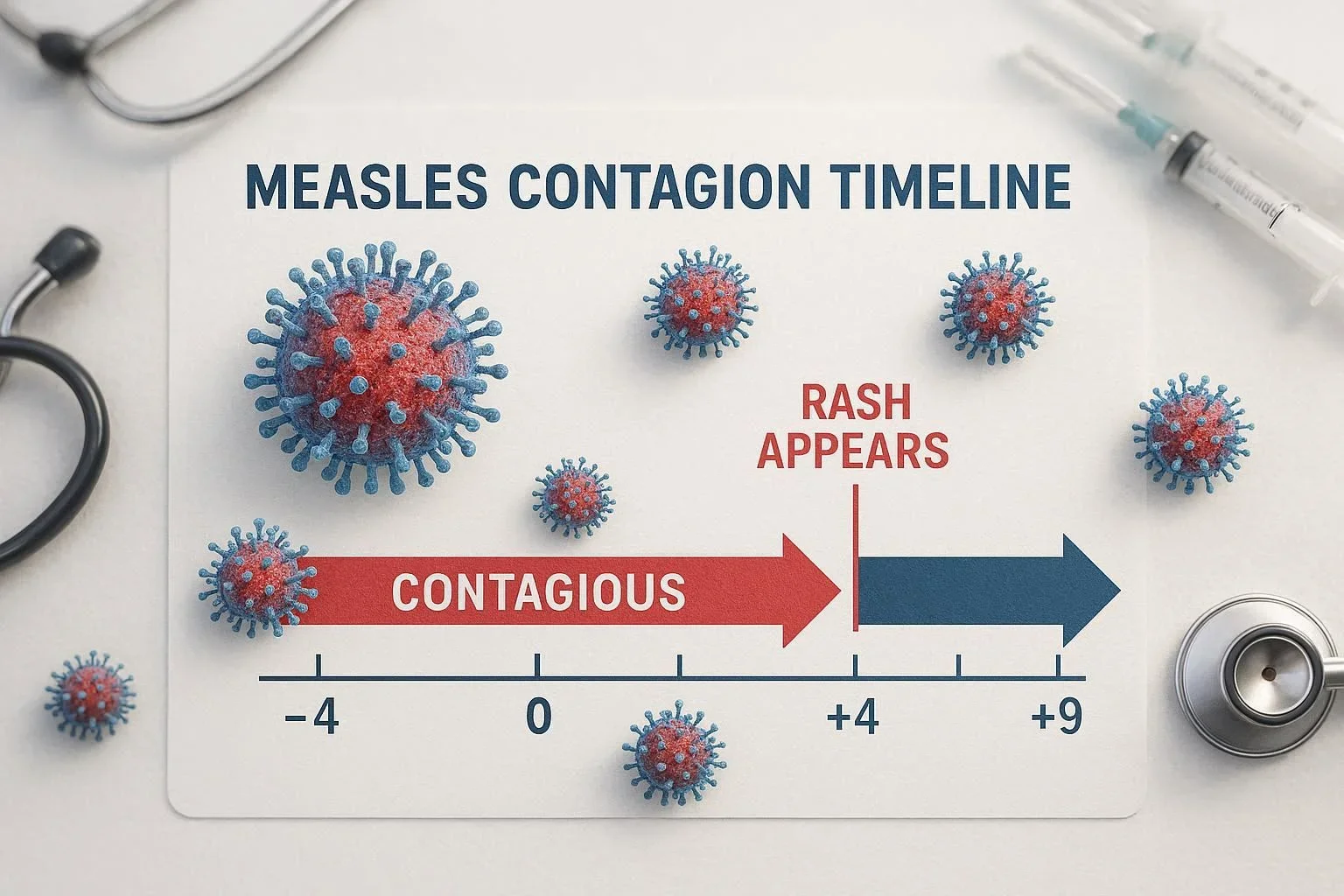
Understanding Measles: Symptoms, Rash, and Contagion Timeline
Initial Measles Symptoms and Infectious Period
Measles is notorious for being highly contagious, often spreading swiftly before a diagnosis is even confirmed. Early symptoms resemble a common cold and typically include fever, cough, runny nose, and red eyes.
Within a few days, many patients develop unique Koplik spots—tiny white spots inside the mouth—that are a classic but not always recognized marker of measles infection. Soon after, the signature measles rash begins, usually starting on the face and then spreading downward.
Surprisingly, an infected person can begin virus transmission four days before the rash appears, contributing to unnoticed community spread. Health experts emphasize that during these early stages, individuals are already a risk to others. This early contagious period is why measles outbreaks can expand rapidly, especially in communities with lower vaccination coverage.
In the days leading up to the rash, an infected person’s coughs and sneezes can release aerosolized droplets containing the virus. These droplets linger in the air or settle on surfaces, remaining infectious for several hours.
According to public health department data, the air in a room previously occupied by a measles patient can still infect others even after the person has left. Given measles’ status as a contagious disease, understanding when transmission begins is crucial for effective public health interventions and outbreak containment.

For a deeper look at how measles outbreaks affect communities and what public health officials are doing to respond, you may find it helpful to review current trends in measles outbreaks and travel safety recommendations. This resource offers practical insights into containment strategies and the broader impact of recent cases.
How Long is a Person Contagious with Measles After the Rash Appears?
The central question—how long is a person contagious with measles after the rash appears—demands precise understanding due to its impact on isolation and public health decisions. Measles patients remain highly infectious for a period that starts four days before and continues until four days after the appearance of the rash. This means that even after the visible symptoms arise, close contacts and household members are still at elevated risk of contracting the illness.
"A person with measles is usually most contagious four days before and four days after the rash appears." — Dr. Emily Carter, Infectious Disease Specialist
Experts reiterate that applying the “four days after rash” rule is based on extensive epidemiological evidence. Measles virus particles are present in an infected person’s respiratory secretions and can be expelled through coughing or sneezing even when the patient feels the worst of their symptoms.
The persistence of contagiousness during this window is why immediate isolation and public notification are always recommended upon suspected or confirmed diagnosis, as per CDC guidance. These precautions help dramatically reduce the risk of spreading the infection, especially in community settings such as schools, clinics, or childcare centers.
Key Facts: How Long a Person Is Contagious with Measles After Rash Appears
Comparison Table of Contagious Periods Before and After Rash Onset
Stage |
Contagious? |
Duration |
|---|---|---|
Before Rash |
Yes |
4 days |
After Rash |
Yes |
4 days |
8+ Days After Rash |
No (in most cases) |
Rare past 4 days post-rash |
CDC guidance recommends isolating individuals with measles for a minimum of four days after the rash appears to protect others and prevent super-spreading events.

Is Measles Contagious After the Rash? Exploring Transmission Risks
Duration of Infectiousness: Scientific Evidence
Based on comprehensive studies of measles cases in the United States, the rash’s appearance does not mark the end of the infectious period—rather, it signals the midpoint. People continue to shed virus and pose a transmission risk for four days post-rash, a fact confirmed by decades of data collected by health departments.
Many parents and caregivers mistakenly believe the risk passes with the fading of the rash, but medical science firmly refutes this. The period following rash development is still dangerous for non-immune people, especially young children and those with weakened immune systems. This is why strict adherence to public health isolation guidelines is vital, even after symptoms seem to improve.
"Even after the rash develops, measles remains highly contagious for several days." — Dr. Rachel Lin, Pediatrician
The heightened awareness triggered by the rash can aid containment—schools, clinics, and workplaces are more likely to respond with swift isolation and contact tracing once visible signs emerge. According to the CDC’s official isolation protocols, individuals are generally released from isolation four full days after the rash appears, assuming symptoms are resolving and no complications have arisen. This “four-day rule” serves as the gold standard in preventing ongoing community transmission.
Measles Outbreaks and Current Trends in the United States
Recent Measles Cases and Public Health Response
In recent years, the United States has experienced a marked uptick in measles cases, particularly in areas with declining vaccination coverage. Resurgence has been linked to international travel and gaps in community immunity, posing challenges for public health officials striving to maintain measles elimination. Notably, outbreaks have been documented in clusters of unvaccinated schoolchildren and among international travelers returning from regions where measles remains endemic.
The CDC and local health departments coordinate measles outbreak responses involving rapid contact tracing, quarantine protocols, and public health education to control measles cases. Increased community awareness of how long is a person contagious with measles after the rash appears is key to halting transmission chains before they reach vulnerable groups, such as young children or immunocompromised individuals.

Prevention: Dose of MMR, Measles Vaccine, and Immunization Strategies
Who Needs a Dose of MMR Vaccine or Measles Vaccine?
The two-dose MMR vaccine, including the essential dose of MMR vaccine, remains the frontline defense against measles infection and measles outbreaks. Young children are recommended to receive their first dose of MMR vaccine at 12–15 months and a second dose at 4–6 years of age.
In measles outbreak situations or before international travel, health authorities often recommend an additional dose of measles vaccine or a dose of MMR vaccine for infants as young as six months and adults without full immunity.
Specific populations—such as international travelers, college students, healthcare workers, and individuals in outbreak-affected communities—may need an extra dose of MMR for optimal protection. The live vaccine approach is highly effective in inducing lasting measles immunity and controlling outbreaks, especially when deployed swiftly after exposure events.

Evidence of Immunity in Vaccinated People and Healthcare Personnel
The concept of evidence of immunity is critical to both personal safety and wider public health strategies. Individuals with written documentation of receiving two doses of a live MMR vaccine, or laboratory proof of immunity, are considered protected—even during outbreaks.
Vaccinated people with evidence of immunity are less likely to develop or transmit measles, thereby protecting vulnerable groups such as young children and those with medical exemptions. Among healthcare personnel, proof of MMR vaccination is typically required as part of infection control standards, dramatically reducing the risk of healthcare-acquired transmission.
Why MMR Vaccination Protects Against Measles
"The best defense remains two doses of the MMR vaccine, which is safe and highly effective." — Dr. Samuel Greene, Epidemiologist
Extensive clinical trials and real-world evidence confirm that two doses of the MMR vaccine provide over 97% protection against measles infection, supporting measles elimination efforts. This strong efficacy underpins measles elimination campaigns worldwide. For maximum impact, communities must sustain high vaccination coverage, especially among young children and populations at greater risk due to frequent international travel or workplace exposures.

Case Study: Managing Measles Exposure and Quarantine Protocols
How Long Do You Have to Quarantine if Exposed to Measles?
After a confirmed exposure, the recommended quarantine duration depends on vaccination status and age. Unvaccinated individuals, including young children and susceptible adults, are advised to quarantine for 21 days following exposure, per CDC and WHO public health guidelines.
This window covers the full incubation period (the time from exposure to symptom onset), which is typically 7 to 21 days. During a measles outbreak, health departments frequently enforce this measure to break the transmission chain. If a potential contact develops symptoms, immediate isolation and medical evaluation are critical to minimize additional spread.
Household contacts are especially at risk due to prolonged and close interactions with an infected person. Even fully vaccinated persons should self-monitor and consult with their healthcare provider upon possible exposure, though they are unlikely to require long quarantines.

Healthcare Personnel and International Travel Considerations
For healthcare personnel, maintaining up-to-date MMR vaccination and evidence of immunity is critical to prevent measles transmission in clinical settings. Unvaccinated or non-immune staff are required to remain away from patient care for the full 21-day period post-exposure or until immunity is documented.
Special travel advisories emphasize that anyone planning international travel to regions with active measles cases must have completed the two-dose MMR vaccine series to reduce infection risk. The CDC provides targeted MMR vaccination guidance for travelers, students, and outbreak-affected populations.
Quarantine Recommendations by Age, Vaccination Status, and Exposure
Group |
Vaccinated? |
Quarantine Required? |
Duration |
|---|---|---|---|
Young children (under 5) |
No |
Yes |
21 days |
Adults |
No |
Yes |
21 days |
Healthcare Personnel |
No |
Yes/Work exclusion |
21 days or until immune |
Fully Vaccinated |
Yes |
Typically No |
Self-monitor |
"Effective containment hinges on timely quarantine and vaccination for those not immune." — Dr. Alana Pierce, Public Health Official
National and international guidelines reinforce that immediate action, clear public messaging, and meticulous implementation of quarantine and immunization can quickly halt measles outbreaks. These best practices have saved lives and reduced severe complications and death from measles worldwide.
Common Myths and Facts: Measles Transmission and Contagion After Rash
Myth: Measles cannot be spread after the rash appears. Fact: Measles is highly contagious for four days after the rash begins.
Myth: Isolation is unnecessary after developing a rash. Fact: Isolation is critical to prevent further transmission for at least four days after rash onset.

Complications: Can Measles Cause Tonsillitis and Other Issues?
Medical studies reveal that while it is rare, measles can cause complications such as tonsillitis, particularly in young children with developing or compromised immune systems.
"While rare, measles can contribute to complications like tonsillitis, especially in young children." — Dr. Laura Singh, Pediatric Infectious Disease Specialist
In addition to sore throat and tonsillitis, measles can lead to ear infections, diarrhea, pneumonia, and—most seriously—encephalitis or brain swelling. Prompt vaccination and post-exposure interventions significantly lower the risk of these serious health outcomes.
Animated breakdown of measles infection stages and contagious period: This educational video walks you through the timeline from exposure through the rash phase, clearly showing when individuals are infectious and highlighting key points for public safety and isolation.
Expert recommendations on vaccination and public health: Learn why vaccination protects both the individual and the wider community, how herd immunity stops outbreaks, and see testimonials from real healthcare professionals and families affected by recent outbreaks.
People Also Ask: How Long Is Measles Contagious and Related Questions
When Are You No Longer Contagious with Measles?
Answer: Typically, you are no longer contagious four days after the rash appears, according to CDC guidelines.
Is Measles Contagious After the Rash?
Answer: Yes, measles remains highly contagious for four days after rash onset.
How Long Do You Have to Quarantine If Exposed to Measles?
Answer: Most public health authorities recommend quarantining for at least 21 days if you are unvaccinated and exposed.
Can Measles Cause Tonsillitis?
Answer: While infrequent, measles can lead to complications such as tonsillitis, primarily in young children.
Key Takeaways: How Long is a Person Contagious with Measles After the Rash Appears
Measles patients are contagious four days before and after the rash.
Timely isolation and vaccination are essential to public health.
Awareness is critical for outbreak prevention.
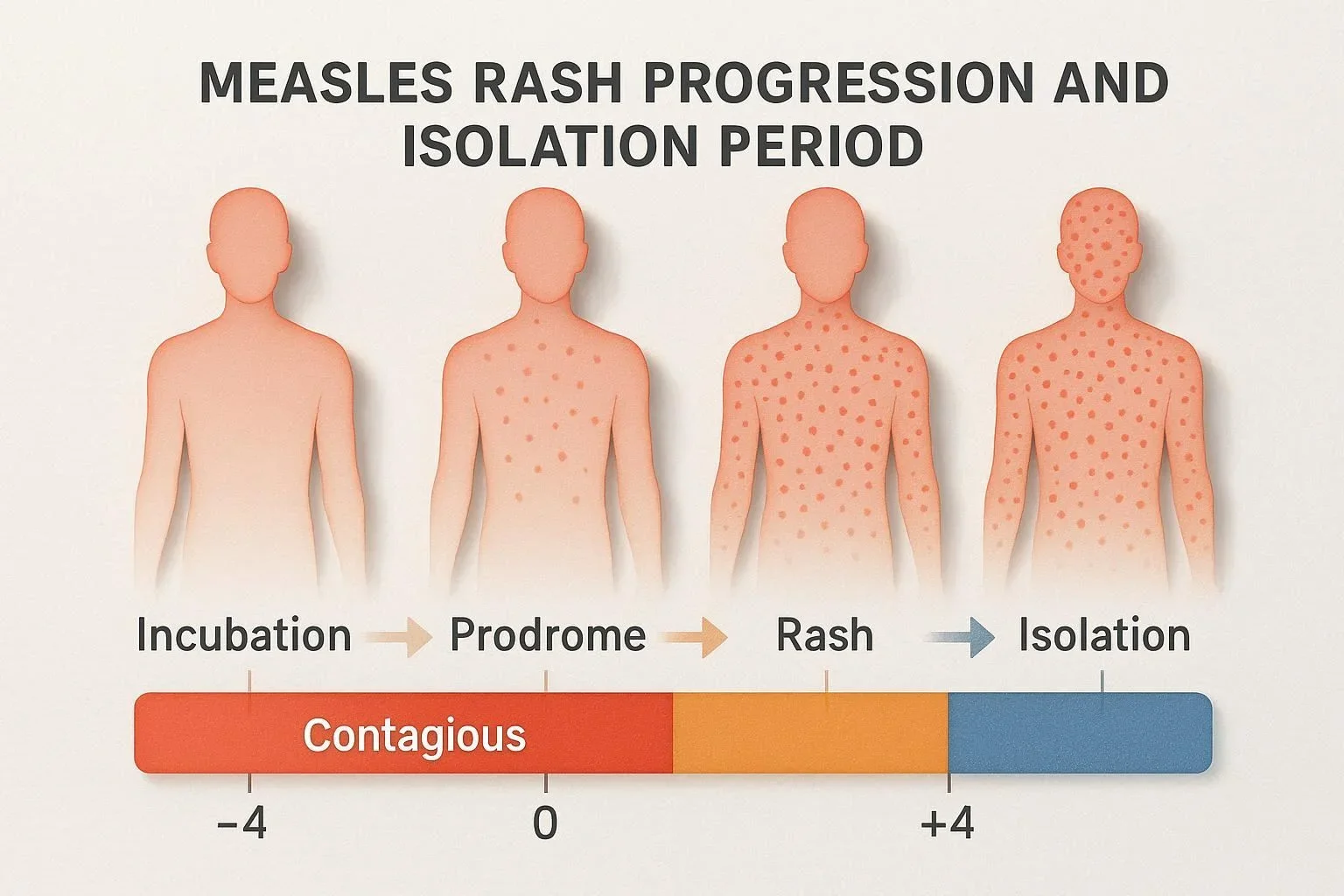
Frequently Asked Questions: Measles Contagious Period and Vaccination
How soon can symptoms start after exposure? Symptoms of measles typically begin 7–14 days after exposure but can start as late as 21 days. The early period includes fever, cough, and Koplik spots before the rash appears.
Does a prior dose of MMR vaccine affect contagiousness? Fully vaccinated people are far less likely to become contagious if exposed, thanks to robust immune system memory from the live vaccine. On rare occasions, mild cases can occur but are typically non-infectious.
What to do if exposed despite prior vaccination? If previously vaccinated, you should self-monitor, consult with your healthcare provider, and notify your health department, but quarantine is not typically required unless symptoms emerge.
Can vaccinated people still spread measles? Secondary transmission from vaccinated people is extremely rare and usually involves only those with incomplete immunity. Full two-dose MMR vaccination provides long-lasting protection for most people.

Final Thoughts and Essential Resources
Stay informed on how long a person is contagious with measles after the rash appears.
Consult your healthcare provider and trusted public health sources for up-to-date guidance.
Learn more about MMR vaccine, outbreak tracking, and measles management at CDC.gov.
If you’re interested in understanding how broader healthcare trends and policy changes can influence disease prevention and community well-being, consider exploring the evolving role of physicians and their impact on public health.
Gaining perspective on the challenges and opportunities facing healthcare professionals can help you appreciate the interconnected nature of outbreak response, vaccination advocacy, and patient care.
By staying informed about both clinical and systemic factors, you empower yourself to make better health decisions and support a stronger, more resilient healthcare system for everyone. NCWellnessHub.com
Conclusion
Understanding and acting on the measles contagious period saves lives—protect yourself and your community by following isolation, vaccination, and public health guidelines.
Sources
WHO – https://www.who.int/news-room/fact-sheets/detail/measles
American Academy of Pediatrics – https://www.aap.org/en/patient-care/measles/
CDC MMR Vaccine Guidance – https://www.cdc.gov/vaccines/vpd/mmr/public/index.html
Understanding the contagious period of measles is crucial for effective prevention and control. According to the Centers for Disease Control and Prevention (CDC), individuals with measles are contagious from four days before to four days after the rash appears. (cdc.gov) This means that even after the rash becomes visible, the person remains capable of transmitting the virus for an additional four days.
The Mayo Clinic also emphasizes that measles can spread very easily, with about 90% of people who haven’t had measles or haven’t been vaccinated becoming infected when around someone with measles. (mayoclinic.org) This highlights the importance of understanding the full contagious period to prevent further transmission.
In summary, a person with measles remains contagious for a total of approximately eight days, spanning from four days before to four days after the onset of the rash. Recognizing this timeline is essential for implementing appropriate isolation measures and protecting public health.
For well-curated articles and expert perspectives, visit: NCWellnessHub.com
 Add Row
Add Row  Add
Add 



Write A Comment