Feeling stuck with constipation is more than uncomfortable—it's frustrating and exhausting. Finding quick, effective relief isn't just a luxury; it's essential for reclaiming your comfort and energy.
Whether you’re experiencing occasional sluggishness or a more persistent problem, understanding what is the best thing for constipation can help you get back to feeling like yourself sooner than you think.
In this comprehensive guide, we’ll walk you through the latest, evidence-backed constipation relief strategies to help restore your digestive wellness—fast.

What You'll Learn: Fast, Effective Constipation Relief Strategies
Top evidence-backed remedies for constipation relief
How dietary fiber, stool softeners, and stimulant laxatives work
When to seek medical help for chronic constipation
Understanding Constipation: Defining the Problem
Overview: What is Constipation and Why Does It Happen?
Constipation is a common digestive complaint that affects millions of people in the United States and worldwide. In medical terms, constipation is typically defined as having fewer than three bowel movements per week, but quality and consistency matter, too.
Common symptoms of constipation include infrequent bowel movements, hard or lumpy stools, straining while using the bathroom, and a sensation of incomplete evacuation. These symptoms may leave someone feeling bloated, sluggish, or even experience discomfort across the digestive tract.
Common symptoms of constipation: infrequent bowel movements, hard stools, and discomfort
Key causes: dietary fiber deficiency, dehydration, low physical activity, certain medications
Difference between occasional and chronic constipation: Occasional constipation is usually short-lived and related to changes in diet, hydration, or routine. In contrast, chronic constipation lasts weeks or longer and may signal an underlying medical condition or persistent lifestyle problem.
Some causes stem from modern dietary habits—many Americans consume far less than the suggested 25–35 grams of fiber a day. Other issues include not drinking enough water (dehydration), a sedentary lifestyle, or as a side effect of certain prescription or over-the-counter medications. For some, chronic constipation may be linked to changes in the digestive system or a medical condition affecting the large intestine or colon.
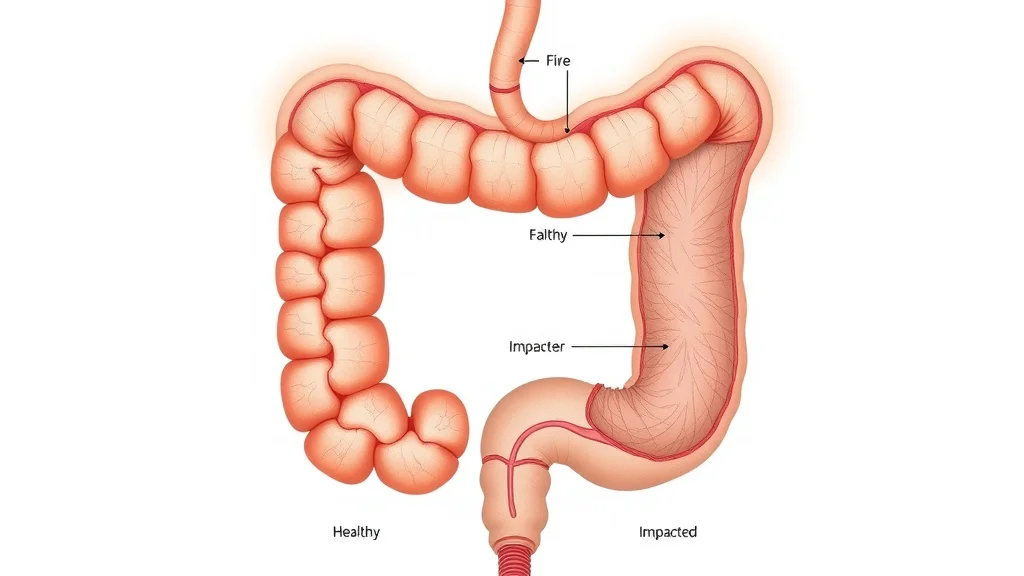
Quick Constipation Relief: What Is the Best Thing for Constipation?
Immediate Constipation Relief: Emergency Remedies
When you’re urgently seeking constipation relief, fast-acting remedies can make all the difference. Over-the-counter (OTC) options like stool softener capsules and osmotic laxatives work by adjusting the way water is absorbed in the digestive tract, making stools softer and easier to pass.
Products such as docusate sodium act as softeners, while polyethylene glycol or magnesium citrate pull water into the colon and quickly ease bowel movements, usually within 12–24 hours. Importantly, hydration is also crucial: drinking 1–2 large glasses of water or a clear fluid can stimulate the digestive system and speed up relief.
Fast-acting over-the-counter options: stool softeners and osmotic laxatives
Hydration and high-volume fluids
“A rapid-acting osmotic laxative, such as polyethylene glycol, can relieve most cases within 24 hours.” – Dr. Kendra Leong, Board-Certified Gastroenterologist
Table: Comparison of Remedy Speed, Effectiveness, and Side Effects
Remedy |
Speed |
Effectiveness |
Possible Side Effects |
|---|---|---|---|
Osmotic Laxative (Polyethylene Glycol) |
6–24 hours |
High |
Bloating, gas, mild cramps |
Stool Softener (Docusate) |
12–72 hours |
Moderate |
Rare (nausea, cramps) |
Stimulant Laxative (Senna, Bisacodyl) |
6–12 hours |
High |
Abdominal cramps, possible dependency |
Warm Fluids (Water, Prune Juice) |
30–120 minutes |
Moderate |
Low risk |
Best Home Remedies for Constipation Relief
For those seeking to relieve constipation at home, evidence points to several safe and effective solutions. Warm prune juice, for instance, contains natural sorbitol—an unabsorbed sugar with a gentle laxative effect—and can speed up a sluggish bowel movement within a few hours.
Increasing your intake of dietary fiber through foods like oats, legumes, fruits, and vegetables helps build stool bulk, while soluble fiber absorbs water, making stool softer and easier to pass.
Warm prune juice and its effect on bowel movement speed
Dietary fiber and soluble fiber sources for sustainable constipation relief
Physical movement and gentle exercise
Adding light physical activity—such as a 10- to 15-minute morning walk—stimulates the digestive system and promotes regular bowel movements. And as Dr. Luis Zedan notes:
“People often overlook the simple power of hydration. Drinking two full glasses of water first thing each morning can assist in regularity.” – Dr. Luis Zedan, Family Medicine Specialist
While dietary fiber is a cornerstone of constipation relief, certain natural supplements may also support digestive health. For example, Colinsonia root has been traditionally used to promote regularity and soothe the digestive tract, offering another gentle option for those seeking holistic approaches.

Exploring Dietary Approaches: The Role of Fiber in Preventing and Treating Constipation
How Dietary Fiber Supports Bowel Movement
Dietary fiber is a foundational element for both preventing and treating constipation. There are two main types of fiber—soluble fiber and insoluble fiber. Soluble fiber absorbs water and forms a gel-like substance in the gut, softening stool and making it easier to pass.
Common sources include oats, beans, lentils, apples, and citrus fruits. Insoluble fiber doesn’t dissolve in water and instead adds bulk to stool, helping food pass more quickly through the digestive tract; good sources are whole wheat bread, brown rice, carrots, and leafy greens.
Difference between soluble fiber and insoluble fiber
List of fiber-rich foods including oats, legumes, fruits, and vegetables
Typical recommended daily fiber intake
The American Heart Association recommends an average of 25–35 grams of fiber a day for adults—yet studies show most people in the United States consume much less. Increasing your fiber intake gradually, while drinking plenty of water, can make a significant difference for sustainable constipation relief and regular bowel movements.

Choosing the Right Fiber for Constipation Relief
Balanced intake of both soluble fiber and insoluble fiber is key to effective constipation management. Soluble and insoluble fibers each play unique roles: one absorbs water to soften stool, the other adds bulk, making stools easier to pass. If you rapidly increase your fiber intake, you may experience side effects such as bloating or excessive gas—avoid this by adding fiber gradually and increasing water consumption alongside it.
How to balance soluble fiber and insoluble fiber
Potential side effects of suddenly increasing fiber
Chart: Soluble Fiber vs Insoluble Fiber: Food Sources and Effects
Type |
Best Sources |
Main Benefits |
Potential Side Effects |
|---|---|---|---|
Soluble Fiber |
Oats, beans, apples, citrus, chia seeds |
Absorbs water, softens stools, lowers cholesterol |
Gas, bloating if intake increases too fast |
Insoluble Fiber |
Whole wheat bread, brown rice, carrots, spinach |
Adds bulk, promotes regular movement |
Cramping, gas if overconsumed without water |
Medical Treatments: OTC and Prescription Options for Constipation Relief
Stool Softeners and Osmotic Laxatives
When home remedies don’t provide enough constipation relief, OTC treatments like stool softeners and osmotic laxatives are a safe next step for most adults. Stool softeners work by moistening the stool, making it softer and easier to pass.
Osmotic laxatives (like polyethylene glycol or milk of magnesia) help retain water in the colon, drawing fluid into the digestive tract so stool moves out easily. It’s important only to use stimulant laxatives (such as senna or bisacodyl) for short periods; prolonged use can cause dependency or worsen symptoms.
How stool softeners work and when to use them
Osmotic and stimulant laxatives: safety protocols, possible risks, and when to stop taking
Always read directions carefully and stop taking stimulant or osmotic laxatives if you develop cramping, severe diarrhea, or dehydration, and consult a healthcare provider for guidance.
Prescription Medications for Chronic Constipation
Persistent or chronic constipation may require medical evaluation, especially if you don’t respond to traditional remedies or if constipation is accompanied by severe pain, rectal bleeding, or a known medical condition. Health professionals may prescribe medications like lubiprostone, linaclotide, or plecanatide—drugs designed to stimulate secretion and movement in the large intestine and colon to restore more regular bowel movements. Each carries potential side effects, including diarrhea and abdominal discomfort, so close monitoring is essential.
When to seek a medical provider for persistent symptoms
Common prescription solutions and side effects
“For longstanding issues, drugs such as lubiprostone or linaclotide may restore regularity where OTC options fail.” – Dr. Sarah Webb, Internal Medicine
Watch:
Lifestyle Changes: Prevent Constipation with Daily Habits
Establishing Healthy Bowel Movement Routines
Forming strong daily routines is one of the most effective ways to prevent constipation and encourage regular bowel movements. Scheduling a few quiet minutes in the bathroom shortly after waking or after breakfast helps train your digestive system to expect predictable output times. Pay attention to your body’s natural urges—ignoring the sensation to go can actually lead to a slower or more difficult to pass stool.
Morning bathroom scheduling tips
Recognizing and acting on natural urges

Physical Activity and Hydration
Staying active and maintaining proper hydration are critical for digestive health. Aim for at least 20–30 minutes of gentle physical activity, such as walking, cycling, or stretching, most days of the week to help stimulate gut movement and relieve constipation. Ensure you’re consuming adequate fluids—ideally at least 8 cups of water per day, and more in hot weather or with increased physical activity.
Recommended activity levels for gut stimulation
Hydration targets and best practices

People Also Ask: Quick Answers to Common Constipation Relief Questions
What is the fastest thing to relieve constipation?
Enemas, stimulant laxatives, and hydration offer the quickest results but should be used with caution. Enemas and stimulant laxatives can quickly trigger a bowel movement—sometimes within minutes to a few hours—but frequent use may lead to dependency or irritation. Opt for these only when immediate relief is necessary and always follow package or medical instructions to ensure safety.
What is the best drink for constipation?
Warm prune juice, water, and magnesium-rich mineral water are among the top evidence-based choices for constipation relief. Prune juice provides sorbitol, a natural sugar alcohol with mild laxative action, while water and mineral water help hydrate the colon and soften stool for easier passage.
What is the fastest for constipation?
Rectal enemas and fast-acting oral stimulant or osmotic laxatives are generally the fastest interventions for severe constipation. Always use under guidance or per instructions to avoid complications, and stop taking them if you experience unusual side effects or if results are not achieved promptly.
What empties your bowels immediately every morning?
A combination of warm fluids like prune juice or water, light stretching, and keeping a consistent morning routine can trigger early bowel movements. With practice, you can help your digestive system establish a rhythm that supports regularity.
Watch:
Lists: Step-by-Step Solutions to Relieve Constipation
Drink 1–2 glasses of water upon waking
Try warm prune juice or a magnesium supplement
Add dietary fiber through oats, beans, and vegetables
Engage in gentle morning physical activity
Only consider OTC laxatives for short-term use after other measures

FAQs: What Is the Best Thing for Constipation?
How does medication affect constipation relief?
Medications—both prescription and over-the-counter—can either relieve or worsen constipation. For some, painkillers, iron supplements, or certain antidepressants make constipation more likely. Always discuss side effects and remedies with your care professional before starting something new, and use laxatives responsibly to treat constipation.Can chronic constipation signal a more serious health issue?
Yes. While most constipation cases are temporary, chronic constipation can point to a more serious digestive or medical condition, such as irritable bowel syndrome, hypothyroidism, or even colon cancer. If you experience unexplained weight loss, blood in your stool, or persistent symptoms despite lifestyle changes, consult a healthcare provider right away.Are natural remedies always safe for everyone?
Natural remedies like dietary fiber and prune juice can benefit most healthy adults. However, those with underlying digestive system conditions—such as inflammatory bowel disease or recent abdominal surgery—should get advice from a health professional before making major changes to their routine.When is it time to see a healthcare provider for constipation relief?
If you have constipation that lasts more than two weeks, experience severe pain, or notice warning signs like blood in the stool, weight loss, or vomiting, it's important to contact a healthcare provider. They can help identify underlying causes and develop a safe, effective treatment plan.
Key Takeaways: Effective, Safe Constipation Relief at a Glance
Hydration and dietary fiber are first-line, sustainable choices to relieve constipation
For fast relief, stool softeners and stimulant laxatives are effective—use only as directed
See a provider for ongoing or worsening chronic constipation
Simple lifestyle shifts can aid both prevention and relief
Constipation relief is achievable for most people when guided by evidence and expert advice. With the right blend of hydration, fiber intake, and timely use of remedies, you’ll reclaim healthy digestion and daily comfort. For personalized strategies, consult your healthcare provider today.
If you’re interested in taking your digestive health even further, consider how fiber-rich foods not only support regularity but also play a vital role in heart health and overall wellness. Exploring the broader benefits of a high-fiber diet can empower you to make choices that protect your cardiovascular system while keeping your digestion on track. For a deeper dive into how these foods can help prevent heart disease and enhance your long-term health, discover the powerful connection between fiber and heart disease prevention. Small, consistent changes today can yield lasting benefits for your entire body.
Sources
Mayo Clinic – https://www.mayoclinic.org/diseases-conditions/constipation
National Center for Biotechnology Information – https://www.ncbi.nlm.nih.gov/books/NBK243/
Gastroenterology – https://www.gastrojournal.org/article/S0016-5085(18)30146-2/fulltext
To enhance your understanding of effective constipation relief strategies, consider exploring the following authoritative resources:
“Constipation Relief: Quick Home Remedies” (healthline.com)
This comprehensive guide outlines various home remedies for constipation, including dietary adjustments, hydration tips, and over-the-counter options.
“Home Remedies for Constipation | Temple Health” (templehealth.org)
This article provides doctor-approved natural methods to alleviate constipation, emphasizing the importance of fiber intake, hydration, and physical activity.
If you’re serious about finding effective and evidence-based solutions for constipation relief, these resources will offer valuable insights and practical tips to help you achieve digestive wellness. NCWellnessHub.com




Write A Comment