Tired of rubbing your eyes and wondering, why are my eyes always itchy? Discover what’s causing this irritation and how to soothe your symptoms effectively
Why Are My Eyes Always Itchy? Opening Insights and Key Causes
Tired of rubbing your eyes and wondering, why are my eyes always itchy? Discover what's causing this irritation and how to soothe your symptoms effectively. Understanding the root can finally give you the relief you deserve—let's explore the answers together.

Many people struggle with itchy eye sensations and wonder, “Why are my eyes always itchy?” Several key causes can trigger this irritating symptom—including seasonal allergies, dry eye, poor contact lens care, or even underlying health issues
What You'll Learn About Itchy Eyes
Overview of why are my eyes always itchy and common causes
Effective remedies for itchy eyes
When to consult a specialist for eye itch
Evidence-based, expert-backed tips on eye health
"Persistent itchy eyes can be caused by multiple triggers—it’s crucial to identify the root cause to ensure proper treatment." — Dr. Maya Sanderson, Ophthalmologist
Understanding Itchy Eyes: Causes, Symptoms & How They Relate to Why Are My Eyes Always Itchy
One of the most common reasons people visit an eye doctor is the frustrating question: why are my eyes always itchy? Understanding the causes gives you the insight needed to choose the right treatment and, just as importantly, prevent further discomfort
The upshot? A thorough understanding of these causes means you can take steps to address the root—not just the symptoms
In addition to these common triggers, your daily environment can play a surprising role in eye irritation. For a deeper look at how indoor air quality and hidden household pollutants may be affecting your eyes, explore the insights in this guide to invisible threats in your home's air. Understanding these factors can help you create a healthier space and reduce persistent eye discomfort.
Common Causes of Itchy Eyes
Environmental allergens (seasonal allergies, dust, pet dander)
Dry eye and dry eyes syndrome
Contact lens and contact lenses use
Eye infections and pink eye
Chronic health conditions (e.g., allergic conjunctivitis)
Table: Common Causes of Itchy Eyes & Associated Symptoms
Cause |
Associated Symptoms |
|---|---|
Seasonal Allergies |
Redness, watery eyes, itchy eyes, sneezing, runny nose |
Dry Eye Syndrome |
Burning, gritty sensation, light sensitivity, eye itch, blurred vision |
Contact Lens Use |
Irritation, dryness, blurry vision, increased eye itch, discomfort |
Eye Infections (Pink Eye, Conjunctivitis) |
Redness, discharge, crusting, swelling, itchy eye, sensitivity to light |
Chronic Health Conditions |
Persistent redness, swelling, eye itch, possibly watery or dry eyes |
"Dry eyes are now one of the leading reasons patients ask me, 'why are my eyes always itchy?' especially with increased screen time." — Dr. Luis Navarro, MD, Eye Specialist
Identifying Your Symptoms: Is It Itchy Eye, Eye Itch, or Itchy Eyes?
Distinguishing between various causes of itchy eyes—like dry eye syndrome, infections, or allergies—can be tricky, but getting it right is crucial for effective relief. Understanding whether you’re dealing with one-off irritation (itchy eye), frequent eye itch, or ongoing itchy eyes helps inform which remedies, prevention strategies, and possible doctor visits you may need. Each trigger manifests with a unique symptom set, from redness to discharge or persistent dryness.
Situational clues are also telling: Do your eyes itch most after spending time outdoors (pointing to seasonal allergies), after screen time (suggesting dry eyes), or while wearing contact lenses (raising the possibility of poor lens hygiene or intolerance)? Knowing these differences will steer you toward targeted solutions, whether it’s eye drops, allergen avoidance, or more robust medical treatment
Recognizing Differences Between Dry Eye, Eye Infections, and Seasonal Allergies
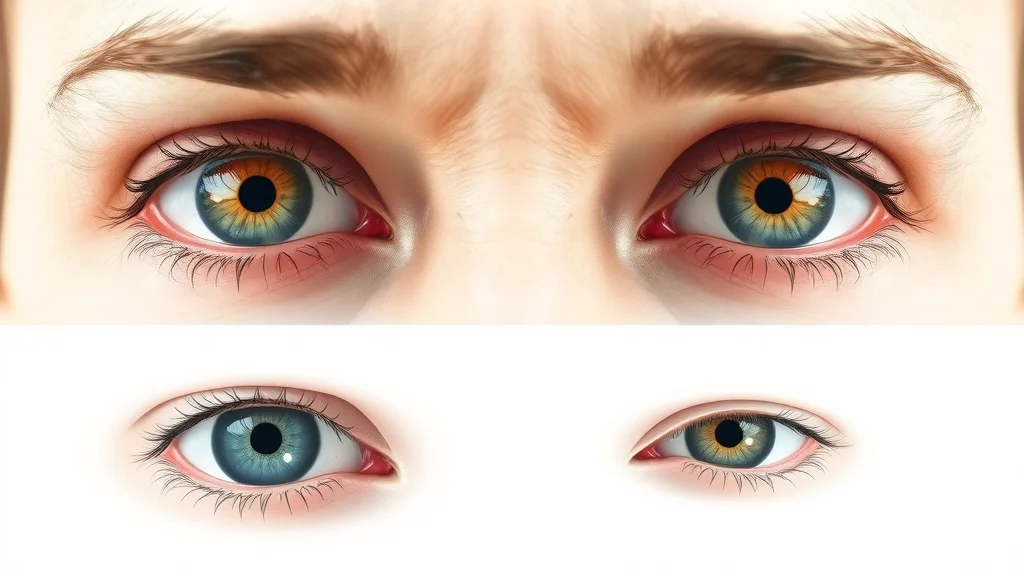
While all of these problems cause eye itch, their presentations vary. Dry eyes typically come with a sand-like or burning feeling and worsen with screen time or in dry environments. Seasonal allergies make eyes red, watery, and are often paired with sneezing or a runny nose, while eye infections (like conjunctivitis or pink eye) frequently bring a sticky discharge and swelling. If your itchy eye comes with intense pain, vision loss, or persistent redness, don’t hesitate to consult an eye doctor for a thorough evaluation.
Red, itchy eyes with crusty discharge? Eye infections like pink eye are likely
Associated Symptoms: Redness, Swelling, Discharge and When to Worry
Redness & Swelling: Indicates inflammation, often seen in allergies and infections.
Discharge: Thick, colored discharge points to infection, while clear discharge may be allergy-related.
Persistent Itching: Ongoing itch with no clear trigger may signal chronic dry eye or an underlying health condition.
Vision Changes: Any vision loss or blurring alongside itchiness requires immediate eye care.
"Itchy eyes from allergies often come with sneezing or a runny nose, while itchy eyes from an infection are usually paired with discharge." — Dr. Elaine Park, Allergist
Environmental and Lifestyle Triggers Behind Why Are My Eyes Always Itchy
Your surroundings play a huge role in why your eyes itch—from pollen outdoors to dust mites indoors and even the air quality after a windy day. Simple lifestyle choices and daily habits can either soothe your itchy eyes or make symptoms worse. Understanding these triggers empowers you to take immediate action for relief.
Common environmental culprits include seasonal allergies, exposure to smoke or chemical fumes, pollution, and extended exposure to air conditioning or heating (which dries out your eyes). Pet dander is another cause, especially for people with indoor animals. Adopting a few practical habits—like using high-efficiency air filters, washing your hands and face after being outdoors, or wearing sunglasses in high pollen environments—can go a long way toward minimizing your risk.
Seasonal Allergies and Allergic Conjunctivitis
Seasonal allergies are one of the top reasons people experience persistent eye itch. When pollen counts rise in spring and autumn, your immune system may overreact, causing watery, red, or itchy eyes. Allergic conjunctivitis is the medical term for this seasonal response affecting the thin membrane covering your eyeball and inner eyelid. The best solutions are limiting exposure to triggers by staying indoors on high-pollen days, using allergy-proof bedding, and keeping windows closed during peak seasons.
Even short exposures to pollens or mold can irritate your eyes and make the symptoms last for days. Over-the-counter antihistamine eye drops and oral allergy medications bring relief, but for some, prescription treatments or referral to an allergist might be needed, especially with severe symptoms.
Impact of Weather, Pollutants, and Lifestyle on Eyes Itch
Tips to reduce exposure to common allergens

Weather shifts—like dry winter air or windy spring days—exacerbate dry eye and increase allergens that irritate your eyes. Pollution and smoke can trigger allergies or cause direct irritation to the sensitive outer layer of your eye. Small adjustments, like replacing home air filters regularly, running a humidifier, or taking breaks from screens, dramatically reduce eye itch. Lifestyle matters, too: For instance, avoid touching or rubbing your eyes, as this worsens irritation and risks introducing bacteria.
Seek out sunglasses with broad coverage when outdoors, keep indoor spaces clean, and try allergy-proof covers on bedding and upholstery. These simple strategies act as a frontline defense against daily environmental offenders. If you notice patterns with specific activities or in particular rooms, track your triggers in a journal to help steer clear of what makes your itchy eyes flare up.
Contact Lens and Eye Itch: How Contact Lenses Cause Itchy Eyes
If you often ask, “Why are my eyes always itchy while I wear contact lenses?” the answer could be as simple as improving your lens care routine or choosing a different contact lens material
Knowing when to replace your contacts, using appropriate cleaning solutions, and practicing better hygiene can transform your eye comfort. Switching to daily disposable lenses or giving your eyes a break by wearing glasses a few days a week may prevent chronic symptoms. Consult your eye doctor for suggestions tailored to your vision needs and eye health.
Contact Lens Hygiene and Preventing Dry Eye

Proper lens care is non-negotiable for anyone who wears contact lenses. Always wash hands thoroughly before touching lenses or your eyes, use sterile solution for cleaning and storage, and never reuse old solution. Replace your case every few months to stave off bacteria. Neglecting lens hygiene can quickly lead to dry eyes, lens intolerance, or an eye infection.
Routinely evaluate the fit and material of your lenses with your optometrist. Some people need lenses made from materials that hold more moisture or reduce protein deposits. If you struggle with eye dryness or itchy eyes despite following a rigorous cleaning routine, talk to your eye care specialist—there may be better options for you, such as scleral lenses or daily disposables.
When to Replace Your Contact Lenses
Overwearing contact lenses is a major cause of itchy eye complaints. Even if your lenses look clean, microscopic deposits and bacteria can remain after each use. Always follow the replacement schedule prescribed—daily for disposables, or as directed for weeklies or monthlies. Never “stretch” lenses for longer use, and always discard any that feel uncomfortable or look cloudy.
If itchy eyes persist after switching to new lenses or following expert advice, schedule a visit to your eye doctor to rule out allergies, dry eye syndrome, or lens intolerance. Leaving a problem untreated can risk more serious issues, such as corneal ulcers or vision loss.
Alternative Vision Correction Options if You Experience Constant Eye Itch
Checklist for Contact Lens Wearers Experiencing Itchy Eyes
If contact lens wear constantly triggers eye itch, ask your optometrist about alternatives. Daily disposable lenses, specialized lens materials (like silicone hydrogel), or switching to prescription eyeglasses even temporarily may provide relief. Some may benefit from refractive surgery or orthokeratology (overnight reshaping lenses) as a long-term answer to frequent itchy eyes.
Use this quick checklist:
Do your lenses still itch after cleaning and replacement?
Have you switched solutions without relief?
Does the problem improve when you stop wearing contacts?
This clarity can help your eye doctor tailor a solution—sometimes changing brands or styles is all it takes to break the itchy cycle

Eye Drops for Itchy Eyes: Best Options and When to Use Them
For many, eye drops provide instant relief for eye itch and dryness. The market is filled with options—including artificial tears, antihistamines, and prescription medications. The key is choosing the type that matches your underlying symptoms and using them as directed.
Selecting the wrong drops can worsen irritation, so always match the formula to your unique complaint. If allergies are your culprit, go for antihistamine eye drops. For dryness from dry eye syndrome, artificial tears are your best bet. Persistent or severe symptoms often require a prescription, so talking with your pharmacist or doctor is always smart.
Over-the-Counter Eye Drop Solutions for Dry Eyes and Eye Itch
Non-prescription eye drops—such as lubricating or artificial tears—work well for mild dryness and irritation. They replenish your eye’s natural moisture, wash away minor debris, and cool burning sensations. Antihistamine or decongestant drops target itchy eyes caused by allergies, reducing both redness and swelling.
Avoid “redness relief” drops containing vasoconstrictors for everyday use, as they may irritate your eyes over time or cause rebound redness. Always check labels and avoid any ingredient you know you’re sensitive to. When in doubt, your pharmacist or eye care specialist can recommend a safe, effective choice.
Prescription Eye Drops and Their Indications
When over-the-counter products aren’t enough, your eye doctor may prescribe stronger eye drops: steroid drops for stubborn allergies, antibiotics for bacterial infections, or immunomodulators for chronic dry eye syndrome. Prescription drops often treat inflammation or address root causes that store-bought solutions cannot.
Always use prescription drops as directed and don’t discontinue use early—even if symptoms improve. Improper use can lead to recurring symptoms or, in some cases, resistance to treatment. If you experience side effects or new symptoms, let your healthcare provider know right away.
Table: Comparing Common Eye Drops for Itchy Eyes
Eye Drop Type |
Best For |
Notes |
|---|---|---|
Artificial Tears |
Dry eyes, general irritation |
Use as needed, safe for most users |
Antihistamine |
Seasonal allergies, allergic conjunctivitis |
Reduces itch and redness, may need daily use |
Decongestant |
Red eye (temporary) |
Not for long-term daily use |
Prescription Steroid |
Severe inflammation, allergies |
Short-term use only, doctor supervision |
Antibiotic Drops |
Eye infection (pink eye, bacterial) |
Must complete full course, prescription only |
"Some eye drops are best for allergies, while others target dry eye. Your symptoms determine the ideal solution." — Dr. Raj Patel, Pharmacist
Medical Conditions That Cause Itchy Eyes: Pink Eye, Eye Infection & More
Sometimes, no matter what you do, your itchy eyes persist. This could be a sign of underlying medical issues, such as pink eye (conjunctivitis), eye infections, or chronic conditions like allergic conjunctivitis and dry eye syndrome. Diagnosing the exact cause is vital, as untreated infections can lead to even more serious problems—including vision loss.
If over-the-counter remedies fail to improve your eye itch, or you’re experiencing additional symptoms—like severe redness, pain, swelling, or vision changes—seek medical attention from your eye doctor or an ophthalmologist immediately. Early intervention preserves both comfort and long-term eye health.
Eye Infections: How to Identify and Treat
Eye infections present as sudden redness, swelling, pain, and sometimes thick or yellowish discharge. These can be viral or bacterial, but either way, prompt professional evaluation ensures safe treatment. Bacterial infections require antibiotic eye drops, while viral forms are usually managed with soothing, supportive care and, in some cases, antiviral or steroid drops.
Never attempt to treat an infection by yourself with leftover medications or home remedies. Improper management can result in more severe symptoms or the spread of infection to others. Practice good hygiene—wash hands often, avoid sharing towels or cosmetics, and see a doctor when symptoms persist.
Pink Eye (Conjunctivitis): Symptoms and Next Steps
Pink eye, or conjunctivitis, is a particularly contagious type of eye infection marked by pronounced redness, gritty sensation, thick discharge, and significant itchy eyes. It can be viral, bacterial, or allergic in origin. Allergic pink eye typically comes with other allergy symptoms, like a runny nose or sneezing.
Treatment depends on the cause, but it almost always involves maintaining strict eye hygiene, avoiding contact lenses during infection, and following prescription instructions carefully. Contact your eye care provider for an accurate diagnosis and targeted treatment—especially if you suspect an infectious cause, to prevent spreading it within your home or workplace.
Chronic Conditions: Allergic Conjunctivitis & Dry Eye Syndrome
Some individuals experience itchy eyes for weeks, months, or even longer; chronic cases often point to allergic conjunctivitis or dry eye syndrome. Allergic conjunctivitis, unlike seasonal allergies, may persist year-round and typically worsens with exposure to triggers like dust, smoke, or animal dander. Dry eye, on the other hand, stems from insufficient tear production or poor tear quality—frequently due to aging, medication side effects, or prolonged screen time.
Long-term relief requires targeted medical intervention—such as prescription lubricating eye drops, allergy management plans, dietary changes, and regular check-ups with your eye specialist. Ignoring chronic eye itch risks potential complications, such as corneal damage or persistent inflammation.
Why Are My Eyes Always Itchy? The Role of Deficiencies and Systemic Health
Your overall health is closely tied to your eye comfort. Deficiencies in key vitamins—such as Vitamin A, Omega-3 fatty acids, and certain B vitamins—can lead to dry eye, itchy eyes, or exacerbate underlying issues. Chronic illnesses (like autoimmune disorders) may also contribute to persistent eye itch. Addressing these systemic factors gives you the best chance at lasting relief.
Regular screenings and blood tests help identify nutritional gaps, while a balanced diet rich in leafy greens, colorful vegetables, and fatty fish supports both eye health and general well-being. Ask your healthcare provider about supplements or dietary modifications if you suspect a deficiency.
What Deficiency Causes Itchy Eyes? Vitamins and Minerals
Common nutritional deficiencies linked to itchy eyes
Lack of Vitamin A is directly linked to dry eyes and surface irritation that causes itchy eyes. Omega-3s help reduce inflammation and improve tear quality, while B12 and folate deficiencies have also been shown to affect tear production and nerve health in the eye. Supplementing your diet under medical supervision may substantially improve symptoms within weeks.
Foods highest in these nutrients include carrots, sweet potatoes, leafy greens, salmon, flaxseed, and walnuts. If symptoms persist despite a healthy diet, a full medical workup is warranted.
How Systemic Health Impacts Ocular Comfort
Conditions like autoimmune diseases, thyroid dysfunction, and diabetes often present with persistent eye itch or dry eye syndrome. Medications—such as antihistamines, diuretics, and antidepressants—may also reduce tear production. Managing these underlying health problems can significantly improve eye comfort and reduce irritating symptoms.
This systems-approach emphasizes the importance of whole-body wellness in the face of ongoing itchy eyes. Engage your general practitioner and eye specialist in your care for comprehensive support.
Table: Essential Vitamins for Eye Health
Vitamin/Mineral |
Role in Eye Health |
Best Sources |
|---|---|---|
Vitamin A |
Prevents dry eye, supports corneal health |
Carrots, sweet potatoes, spinach |
Omega-3 Fatty Acids |
Reduces inflammation, improves tear stability |
Salmon, flaxseed, walnuts |
Vitamin B12 |
Supports nerve health, tear production |
Fish, eggs, fortified cereals |
Vitamin C & E |
Antioxidants for eye tissue repair |
Berries, citrus, nuts |
When Should I See a Doctor for Persistent Itchy Eyes?
Warning signs to watch for
How an eye care specialist can help with why are my eyes always itchy
While mild irritation is common, unrelenting itchy eyes may signal a problem needing medical intervention. Watch for signs like severe redness, vision loss, persistent pain, thick discharge, or symptoms that don’t improve with over-the-counter eye drops. Eye care specialists can run specific tests, pinpoint allergens or infections, and prescribe targeted therapies that bring lasting relief and prevent complications.
"If over-the-counter remedies fail and symptoms persist, seek professional evaluation to prevent vision complications." — Dr. Jasmine Lee, OD
Self-Help and Home Remedies for Why Are My Eyes Always Itchy
Many people find relief with simple home strategies for itchy eyes. Effective self-care includes applying clean cold compresses, frequent hand washing, avoiding known triggers, and using lubricating eye drops as needed. Make sure bedding and home surfaces are kept free from dust or pet dander, and avoid smoky or polluted environments if possible.
Lifestyle adjustments also play a major role. Take regular screen breaks, blink frequently when reading or working at a computer, and maintain a humid environment indoors during dry seasons. Remember, never rub your eyes—it may worsen irritation or transfer bacteria.
Effective Do-It-Yourself Tips for Relieving Itchy Eyes
Try the following at home: Gently place a chilled, clean washcloth over closed eyes to soothe burning and swelling. Use preservative-free artificial tears for dry or irritated eyes several times per day. Avoid makeup or skincare products that irritate your eyes. Change pillowcases and sheets often and use allergy-proof covers if dust or pet dander is a problem.
If symptoms worsen or persist, or if you experience pain or vision changes, seek professional medical evaluation.
Lifestyle Changes for Itchy Eyes Prevention
Step-by-step: Applying cold compresses, maintaining eye hygiene, choosing the right eye drops

Building habits for eye comfort makes a big difference: avoid rubbing your eyes, wear sunglasses outdoors, keep your living space free of allergens, and carefully follow your prescribed eye care routine. Consider using a humidifier during heating season, eat a diet rich in eye-healthy nutrients, and stick to your lens replacement schedule if you wear contact lenses. These small steps combine to dramatically reduce recurrence of uncomfortable eye itch.
People Also Ask About Why Are My Eyes Always Itchy
How do you get rid of itchy eyes?
Learn practical tips for soothing itchy eyes and restoring comfort—from cold compresses to proper eye drop use and allergen avoidance.
To get rid of itchy eyes, start by avoiding triggers such as pollens and pet dander. Apply a cold compress and use over-the-counter lubricating eye drops for rapid relief. Practice good eye hygiene, and keep home surfaces dust-free. If allergies cause symptoms, antihistamine drops may work best. For persistent or severe itch, or if there’s pain or changes in vision, see an eye care specialist.
What deficiency causes itchy eyes?
Vitamin A, Omega-3, and certain B vitamins play a role in eye health—learn how these deficiencies can influence itchy eyes.
Deficiencies in Vitamin A, Omega-3 fatty acids, and B12 are linked to itchy eyes and dry eyes. These nutrients support tear production, reduce inflammation, and protect ocular tissues. If you notice chronic eye irritation alongside other symptoms of poor nutrition, consult a doctor to rule out dietary causes and discuss a supplementation plan.
What condition causes itchy eyes?
Explore health conditions ranging from allergic conjunctivitis to dry eye syndrome and how they can all be responsible for that constant itchiness.
Several health conditions can cause persistent itchy eyes: allergic conjunctivitis (chronic inflammation due to allergies), dry eye syndrome (reduced tear production or poor tear quality), or eye infections like pink eye (conjunctivitis). Other culprits include autoimmune conditions and eyelid inflammation. A thorough evaluation is key to matching the treatment with the underlying cause.

FAQs on Why Are My Eyes Always Itchy, Itchy Eyes, and Dry Eye
-
What are the main reasons for having itchy eyes every day?
Daily itchy eyes are often caused by allergies, dry eye, prolonged screen use, contact lens wear, or environmental irritants.
-
Can screen time make my eyes itch more?
Yes. Prolonged screen time reduces your blinking rate and can cause dry eyes, leading to more frequent eye itch.
-
Do allergies always cause itchy eyes?
Allergies are one of the most common reasons, but not the only cause. Dry eye and infections may also lead to itching.
Are there natural remedies or must I use eye drops?
-
Natural remedies—like cold compresses, air purifiers, and dietary adjustments—can help, but sometimes eye drops or medical treatment are needed for persistent symptoms.

Key Takeaways: Relief and Prevention Strategies for Why Are My Eyes Always Itchy
Most causes of itchy eyes are manageable with proper hygiene, lifestyle changes, and targeted treatments.
Persistent or worsening symptoms require an expert evaluation.
Choose eye drops and remedies based on your diagnosed underlying cause.
Where to Find More Evidence-Based Health Questions & Answers
Discover more trusted information like this at: NCWellnessHub.com
Conclusion: Relief from why are my eyes always itchy is achievable—identify your triggers, practice smart self-care, and seek medical guidance when needed for lasting eye comfort.
If you’re ready to take your eye health to the next level, consider exploring the daily routines and proactive habits that set apart those with consistently healthy eyes. From nutrition to mindful screen use and protective strategies, these expert-backed habits for remarkably healthy eyes offer actionable steps for lasting comfort and clarity.
By integrating these advanced tips into your lifestyle, you can move beyond symptom management and work toward optimal, long-term eye wellness. Your journey to brighter, more comfortable eyes starts with the right knowledge and a commitment to healthy habits. NCWellnessHub.com




Write A Comment